Monkeypox: Q&A and update
Simon Collins, HIV i-Base
This Q&A is about the recent cases of monkeypox virus (MPV) in the UK. It will be updated as new information becomes available.
Monkeypox virus (MPV) is still very rare in the UK. But the recent outbreak is significant though and needs to be taken seriously.
Information is organised into six sections
- MPV basics
- Prevention and transmission
- Testing and treatment
- MPV and HIV
- Other questions
- References and more information
1. MPV: first questions
What is monkeypox?
Monkeypox is an infection caused by the monkeypox virus (MPV).
MPV is usually rarely seen in the UK. However, during May 2022 MPV was reported in 79 people in the UK.
MPV also been reported in about 150 people in other countries. International travel links cases in the UK, Europe, Canada, the US and Australia.
The risk of MPV needs to be taken seriously. This is both for your individual health and so that it doesn’t become an established infection.
Are there different strains of MPV?
Yes. Like most viruses there are different strains of MPV.
The two main strains are a mild form (linked to West Africa) and a more aggressive form (linked to Central Africa).
The current cases all involve the mild version.
What are the main symptoms?
Many of the early general symptoms are similar to other infections like colds, flu and COVID.
These include fever, headache, muscle aches, backache, swollen lymph nodes, chills and feeling very tired.
Sometimes they are mild. Some people do not get these at all.
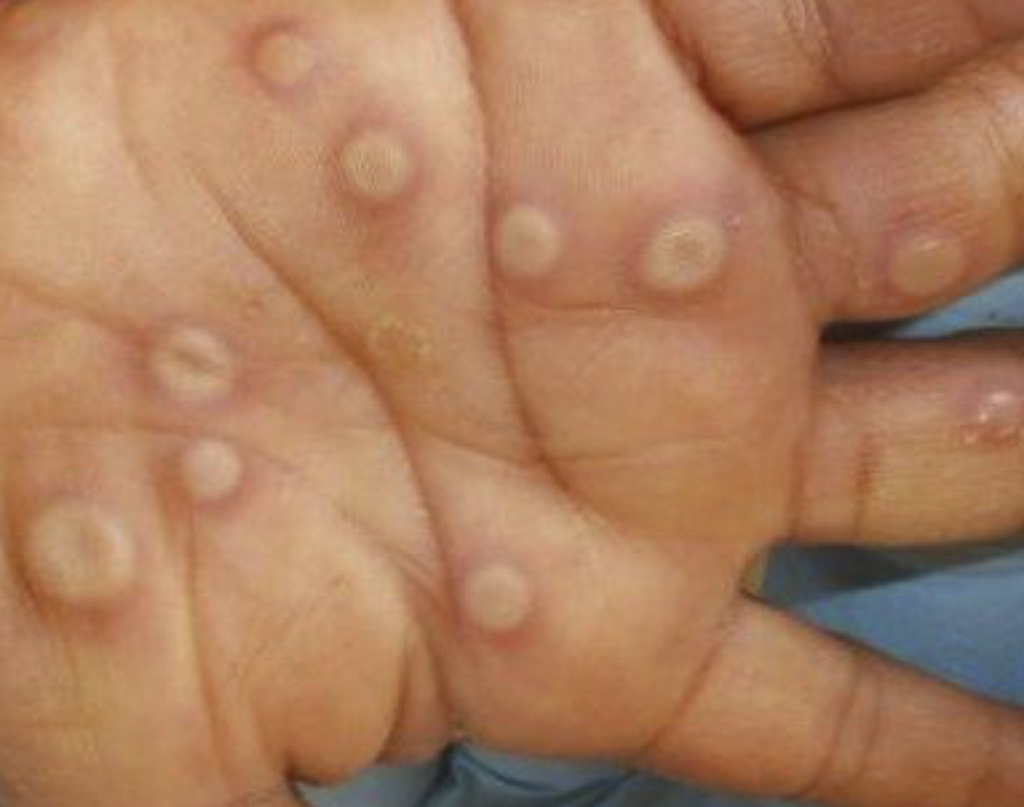
MPV rash develops a few days after the symptoms above. This starts as red skin bumps, often in the genitals or face. It can evolve to fluid filled blisters that can break down into ulcers or sores. These develop into a scab that eventually falls off.
The rash can include any part of the body. The sores can be painful, aggressive and unpleasant. They can also be itchy. Scratching can potentially spread the virus to other sites which could become very serious.
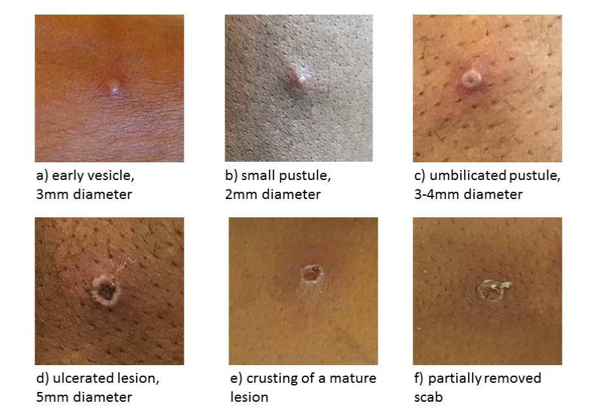
The examples below are the different stages of the rash. The rash can vary in size from a few millimetres to a centimetre in diameter.
How is the MPV rash different?
There are other pictures at this link to the US CDC.
https://www.cdc.gov/poxvirus/monkeypox/clinicians/clinical-recognition.html
- Lesions can be similar to several more common infections. These include chicken pox, syphilis, herpes, molluscum, cryptococcal infection, shingles (VZV) or even some heat rashes.
- Rash with many of these are soft though. MPV lesions are deeper and harder.
- MPV lesions can appear in crops every three to five days, and unlike chickenpox can take several days to evolve into blisters.
- MPV lesions often have a dip in the centre with a dot in the middle. This is called umbilicated.
How serious is MPV?
Most cases are mild.
With support, most people will be able to self-isolate at home.
However, 1 in 100 cases can include serious complications. This can involve inflammation of the lungs (pneumonitis), brain (encephalitis), eyes (keratitis) and bacterial infections.
The sores of MPV can become infected with bacteria, and if untreated appropriately, can lead to septicaemia (blood poisoning).
Serious infections need to be managed in hospital.
Is MPV an STI?
Currently no. MPV is transmitted via close contact, and maybe transmitted via close skin contact, or contact with infected clothes, towels and bed linen or even saliva. Having sex involves close contact.
Sexual contact is not necessary, but lesions in the genital area will be very infectious.
Even if later research finds MPV is infectious in sexual fluids, the larger risk is likely to come from close contact.
Condoms, for example, will not protect against MPV.
However, one exception might be if MPV remains in sexual fluids after the infections is otherwise cleared. Currently, this is not thought likely, but needs further research.
Does MPV just affect gay men?
No, viruses do not care about sexuality.
Recent infections in gay men is because this is one of the networks of an early infection.
2. Transmission and prevention
What is the risk of catching MPV?
So far the risk of catching MPV is very low for everyone. This is because MPV is still rare in the UK.
But knowing about the risk is important in settings where MPV risks are already higher.
- Casual social contact is generally very low risk in all settings.
- But this can be higher with sexual partners and people you live with.
For both reasons, people diagnosed with MPV need to self-isolate until the infection is cleared.
How is MPV transmitted?
MPV can be spread in several ways.
- Through droplets in the air.
This usually involves spending extended time with someone in a room with poor ventilation. For example, spending more than 3 to 6 hours, where you are within two metres.
So casual contact in the same room is a very low risk, unless someone directly sneezes in your face.
But transmission by air is a much higher risk for people in the same household. This should involve taking special precautions to limit contact with people you live with.
- By close contact with someone who has symptoms.
This is especially after the rash has developed. This is because the fluid in MPV lesion will be highly infectious.
Skin contact with lesions is a high risk of catching MPV.
- By sharing sheets and towels.
Sharing sheets and towels with someone with MPV can also be a route of transmission.
Washing sheets and towels can also be a risk. This is in case infectious material is shaken into the air.
A machine wash at a 60 degree cycle will be enough to sterilise sheets, clothes and towels.
Simple cleaning with household bleach will be enough to sterilise surfaces, toilets and bathrooms.
How long after an exposure risk does MPV take to develop?
Based on the limited data, it can take from 1 to 3 weeks until MPV produces symptoms.
For most people this is 10 to 12 days after contact.
When is someone infectious?
The risk of onward transmission starts as soon as there are symptoms.
The risk usually ends after the rash and scabs have gone.
This is why it is important to call a doctor or clinic for advice. But please do not visit a doctor or clinic without calling first so this can be arranged properly.
Otherwise health workers might also need to isolate.
What if I have been exposed to MPV?
Recommendations on recent risk depend on whether the risk is high, medium or low risk.
High risk is defined as close contacts of people who develop MPV. This includes being withing 6 feet for more than three hours, sexual contact or direct contact with body fluids. It can also include contact with shared sheets and towels.
Please self-monitor for symptoms for the next three weeks. This can include taking your temperature twice a day which should stay below 38°C (100.4° F)
Seek medical advice if you develop any of the symptoms above, especially fever, rash, chills or swollen lymph nodes. In the UK this should be by calling a sexual health clinic or by calling 111.
It is important to self-isolate if you develop symptoms and follow health care advice.
People at higher risk might be offered PEP with vaccination. This will usually be from spending prolonged time with someone with diagnosed MPV or direct contact to lesions or body fluids.
Vaccination is usually only offered to people at high risk.
How can I reduce my risk and stay safe?
The current advice for how to reduce your risks is likely to change every week.
This will depend on how successfully MPV is contained or on whether cases continue to rise. This might mean this advice changes, depending on where you live and on different social situations.
This also involves a personal approach to healthcare both for yourself and for the community. For example, to get medical advice if you feel unwell or develop an unexpected rash. This will also help you access the best care to recover quickly.
One of the higher risks comes from contact with sexual partners, So reducing the numbers of partners, especially in a group setting will help. This is especially important at gay and bisexual venues in London.
Social events that involve being with many people for hours in a poorly ventilated space will be a higher risk than outdoor events with fewer people. This is whether or not anyone is having sex.
This will hopefully only for a short time, perhaps only for the next few weeks.
Will having MPV once protect me against catching it again?
Although this might be possible, there is currently not enough information to answers this question.
Even if it is possible, this would not be something to rely on before there is data.
Also, cases have been reported when cases have returned after the infection was thought to be cured. In these cases special tests are need to find out whether or not this is a new infection.
3. Diagnosis and treatment?
What if I have symptoms?
If you are worried about symptoms, please telephone a sexual health clinic (or 111 in the UK).
Contact by phone is important. The clinic will ask you about symptoms, including to describe any rash.
Please do NOT visit the clinic using a drop-in service. This could cause health workers to need to isolate and staffing is already under pressure.
Anyone in the UK can access free testing and treatment at a sexual health clinic.
How is MPV diagnosed?
A distinctive rash appearing a few days after other general symptoms is enough for MPV to be very likely, even before it is confirmed by a test.
This will involve a doctor checking that the rash isn’t another more common infection.
However, testing is still important to rule out other pox viruses.
PCR testing is used to confirm MPV. This involves sending samples to a specialist laboratories.
How important is contact tracing?
Anyone diagnosed with MPV will be asked for details about people they have been in close contact with.
This will help to identify people who might be at risk, and may benefit from PEP.
Effective contact tracing could limit how serious MPV becomes in the UK. It will be done very carefully and sensitively. This is a specialist part of sexual health care.
People who are thought to be at high risk will then be asked to self-monitor for symptoms over the next three weeks. They will be monitored with a daily phone call, and they may be offered vaccination as PEP.
Can MPV be treated?
Yes. Although most people are likely to be monitored without direct treatment.
If needed, several oral drugs are being used to treat MPV, especially if symptoms are more than mild.
These include brincidofovir (once a week) and tecovirimat (twice daily for 2 weeks),
Both these drugs were approved to treat other infections similar to MPV. This means there is little direct evidence about whether they work for MPV.
As most infections are mild, treatment is only offered to more severe cases, or to people at higher risk of severe infection.
This can include people with reduced immune functions, children younger than 8, pregnancy, and selected other infections.
Vaccines are also being used to manage and reduce the risk from infection.
Which vaccines are used against MPV?
Two vaccines against smallpox are currently being used against MPV.
The main vaccine is called Imvanex (also called Imvamune, Jynneos and MVA). It is a live but non-replicating vaccine that is also approved against MPV in the US in 2019. This vaccine is safe to use by people living with HIV. It is given in two doses, 28 days apart.
An earlier vaccine called ACAM2000 was approved in 2007 but is a live replication-competent vaccine. Although it is given as a single dose it is not recommended in people living with HIV.
Are the vaccines effective?
The smallpox vaccine is likely to help even if given after contact. It should limit the risk of infection or limit the severity of illness if the infection develops. This may be up to 85% effective.
Vaccination for close contacts is most effective when given within four days of contact. However, it might still be effective for up to 14 days after.
Will smallpox vaccinations from childhood still be active?
Many adults older than 50 will have had the smallpox vaccine as a child.
It is possible that this may offer some protection against MPV.
Smallpox vaccinations were stopped in the UK in 1971 and immune responses become much lower after 10 years.
4. HIV and MPV
How does HIV affect MPV?
The British HIV Association (BHIVA) published a recent statement on MPV.
This says that HIV should not increase your risk of catching MPV. It also should not make MPV a more serious infection.
This is based on you having an undetectable viral load and a CD4 count that is well above 200 cells/mm3. This is a cautious approach because there is too little direct evidence about this.
Please see this link to BHIVA and ECDC statements about MPV.
https://i-base.info/htb/42896
5. Other questions
What are the differences between MPV and COVID?
Although everyone will worry about the similarities to COVID-19.
There are important differences that will stop MPV from becoming a pandemic.
- MPV only becomes infectious after there are symptoms. COVID was devastating because it was infectious several days before anyone had symptoms.
- MPV is heavier than the COVID virus, MPV is heavier. This makes it more likely to fall to the ground rather than stay in the air.
- COVID infection was through the nose, throat and lungs. Although MPV can be caught from droplets in air in a confined space, but is more commonly caught by physical contact.
- MPV is much less likely to mutate into different strains than COVID.
- COVID was a more severe infection. Many people needed time in intensive care and in the most serious outcomes, people of all ages died.
What about transmission to animals?
This is an important concern with MPV.
Despite the name, MPV is more linked to infections in other animals. This includes in mice, rats and squirrels.
An outbreak in the US in 2003 was linked to prairie-dogs (which are not dogs).
The concern about other animals being carriers for MPV is that this might make it difficult to control the virus in the long-term.
It is also important for people who self-isolate at home to know whether this also needs to be from their pets. Advice was not initially given on this question, However, on 27 May the UK included the need for people diagnosed with MPV to also isolate from their pets. Similar guidance is made by the ECDC.
This is to reduce the risk that animals could become a long-term reservoir for MPV.
Gerbils, hamsters and other rodents have a very high risk of catching MPV. Other pets including cats and dogs should be kept isolated at home. However, it is difficult to set how “regular vet checks to ensure no clinical signs are observed” is expected to work.
While this advice is laudable in the case of pets, the guidance doesn’t extend to unwelcome rodents that are present despite complaining to your landlord. This might however be a fast-track way to prompt a response.
6. References and further information
The following sources were used for the information on this page.
- NHS. Monkeypox.
https://www.nhs.uk/conditions/monkeypox
Non-technical information about MPV in the UK. This includes who to contact if you are worried about symptoms. - UK.gov. Monkeypox virus. (23 May 2022).
https://www.gov.uk/guidance/monkeypox
More detailed information from the UK government about all aspects of MPV including update on the current outbreak. - BHIVA rapid statement on monkeypox virus. (17 May 2022).
https://www.bhiva.org/BHIVA-rapid-statement-on-monkeypox-virus - European Centre for Disease Prevention and Control (ECDC). Monkeypox multi-country outbreak: rapid assessment report. (23 May 2022).
https://www.ecdc.europa.eu/en/publications-data/risk-assessment-monkeypox-multi-country-outbreak (download page)
https://www.ecdc.europa.eu/sites/default/files/documents/Monkeypox-multi-country-outbreak.pdf (PDF)
See also this slide set from an informal webinar given on 24 May 2022.
Monkeypox ECDC webinar (PDF) - Adler H et al. Clinical features and management of human monkeypox: a retrospective observational study in the UK. The Lancet, DOI: 10.1016/S1473-3099(22)00228-6. (May 24 2022).
https://www.thelancet.com/journals/laninf/article/PIIS1473-3099(22)00228-6/fulltext
Details of seven MPV cases reported in the UK between 2028 and 2021. - US CDC. What clinicians need to know about monkeypox in the United States and other countries.
https://emergency.cdc.gov/coca/calls/2022/callinfo_052422.asp
This US talk on clinical management includes pictures of MPV compared to other common rashes. - US CDC. Monitoring people who have been exposed.
https://www.cdc.gov/poxvirus/monkeypox/clinicians/monitoring.html - US CDC. Home page for information for doctors about MPV.
https://www.cdc.gov/poxvirus/monkeypox/clinicians/index.html - International Monkeypox case tracker.
https://monkeypox.healthmap.org - Human Animal Infections and Risk Surveillance group (HAIRS). Qualitative assessment of the risk to the UK human population of monkeypox infection in a canine, feline, mustelid, lagomorph or rodent UK pet. (27 May 2022).
https://www.gov.uk/government/publications/hairs-risk-assessment-monkeypox/qualitative-assessment-of-the-risk-to-the-uk-human-population-of-monkeypox-infection-in-a-canine-feline-mustelid-lagomorph-or-rodent-uk-pet